Many of you can probably relate to either having experienced plantar fasciitis (PF) yourself or perhaps you’ve had a family member, friend, gym buddy, or running mate impacted by this foot pain. That was our motivation behind creating this blog post. To do a deep dive into the literature on PF and provide you folks with some education on the condition as well as what you can do to improve and prevent symptoms.

prevalence
PF is the most common cause of persistent heel pain in adults, making up 10-15% of health care visits for foot symptoms. It is estimated that 1 in 10 people will develop plantar fasciitis in their lifetime.
anatomy
The plantar fascia is the thick connective tissue which supports the arch of the bottom of the foot. It runs from the calcaneus (heel bone) to the heads of the metatarsal bones at the base of your toes. The plantar fascia also plays an important role during gait, behaving like a spring during the stance phase and contributing to the “windlass mechanism” when the toes are dorsiflexed in the propulsive phase.
pathophysiology
The literature suggests that the changes in the plantar fascia are degenerative rather than inflammatory. So we really should be calling it fasciosis (degenerative process) than fasciitis (inflammatory process) but we will put our nerd hat’s down and go forward with the more common name.
risk factors
Risk factors associated with PF can be divided into two groups: intrinsic + extrinsic factors. Intrinsic factors are specific to the individual which are within the body where as extrinsic factors are things within the environment or influences outside of the body which have a contributing effect on the onset of a condition/disease process.
Intrinsic factors associated with PF:
- age
- obesity
- family history
- over pronation/supination of the foot
- decreased toe extension range of motion
- decreased ankle dorsiflexion
Extrinsic factors associated with PF:
- inappropriate footwear
- occupational loads of prolonged standing
- terrain and training surface
- ramping up activities too fast too soon
signs & symptoms
PF classically presents as heel pain + stiffness that occurs with your first few steps in the morning. As you get up and move around it typically subsides, but the pain + stiffness may return after long periods of standing or when you stand up from prolonged sitting.
differential diagnosis
- plantar fascia rupture
- fat pad syndrome
- calcaneal stress fracture
- tumor
- calcaneal bursitis
- boxter’s nerve entrapment
- medial calcaneal entrapment (tarsal tunnel syndrome)
- seronegative arthropathies
- spinal stenosis and L5-S1 nerve root irritation
treatment
Conservative therapy such as chiropractic, physiotherapy, and massage therapy are recommended over more invasive interventions for the treatment of PF. Interventions include: stretching of the plantar fascia and calf muscles, strengthening exercises for foot intrinsics + high load strength training of plantar flexors, night splints, taping, dry needling, and manual therapy techniques like joint mobilization, massage, and active release techniques (ART).
Custom orthotics are also one of many conservative treatment options available for treating PF. These devices are designed to restore functional capacity to the foot, control abnormal motion, reduce stress on soft tissues and help alleviate pressure in the foot. A registered chiropodist can perform an evaluation of your feet and take a cast moulding to manufacture a custom orthotic based on your individual needs.
A combination of manual therapy, education and strength + conditioning should be established with your clinician. Your rehab should also be specific to YOU! Our clinicians at Function101 can determine which risk factors may be driving your pain and help you move forward.
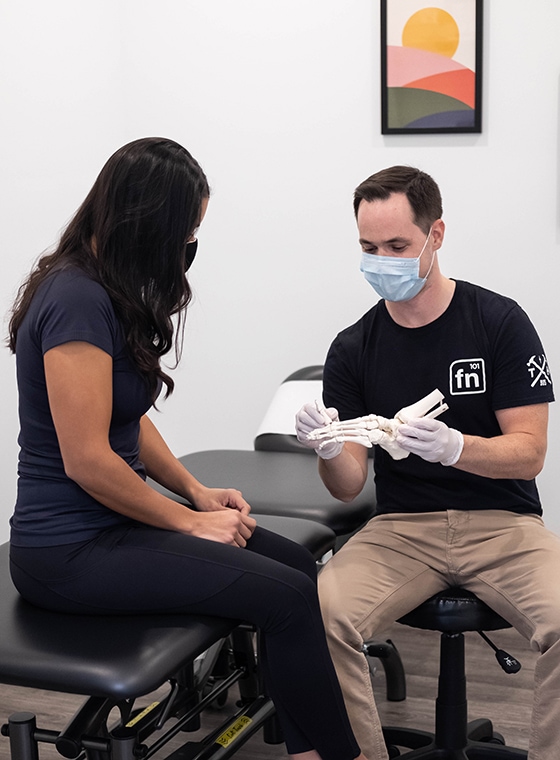
Here are some of the rehab strategies that we use with our clients to help them recover from plantar fasciitis. These exercises fall within 4 main categories:
- pain management
- mobility of great toe + ankle
- strengthening foot intrinsics
- progressive loading of the lower extremity
To keep things simple, we’ve also broken down the rehab into 3 phases of recovery, starting with “101” and progressively loading the tissues to “301” near end stages of rehab.
101
- self massage of plantar fascia + gastroc/soleus complex
- towel PNF stretch of gastroc/soleus
- short foot intrinsic isometrics
- seated bilateral calf raise (loaded with dumbbell)
201
- big toe extension PNF stretch
- short foot toe taps
- split squats with calf raise
- bilateral calf raise with towel under the toes to maximally dorsiflex
301
- modified runners stretch (PNF)
- single leg RDL (short foot cue)
- dumbbell rear elevated split squats
- bilateral calf raise off step with backpack filled with weight/books
Follow us on instagram @function101locke for more educational content!
References:
Bandara EMIA, Kularathne WNI. Physical therapy interventions for plantar fasciitis: a review article. Journal of Advanced Engineering and Science. 2019;4(4): 176-187.
Rupareliya D, Shukla Y, Bhise A, Prabhakar M. To study the effect of eccentric loading exercises of calf muscles in plantar fasciitis. An interventional study. Physiotherapy. 2015;101 (1):E1303-E1304.
Tahririan MA, Motififard M, Tahmasebi MN, Siavashi B. Plantar fasciitis. J Res Med Sci. 2012;17(8):799-804.